Contents
In this article we will look at:
- What is osteoarthritis?
- How does osteoarthritis occur?
- Who is prone to osteoarthritis?
- What are the causes of osteoarthritis?
- What are the symptoms of osteoarthritis?
- How is osteoarthritis diagnosed?
- What are the complications of osteoarthritis?
- What is the treatment for osteoarthritis?
You can click on any of the links above to navigate to the section of your interest.
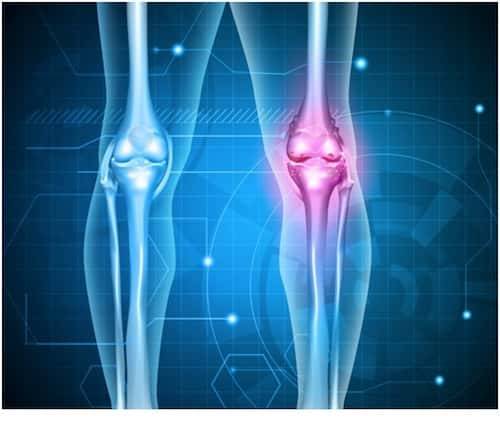
What is osteoarthritis?
Also known as degenerative disease, or degenerative arthritis, osteoarthritis is a chronic condition that affects the joints, which results from results from breakdown of joint cartilage and underlying bone. This is the most common type of arthritis and is seen especially among older people above 50 years of age.
People with osteoarthritis usually suffer from symptoms of joint pain and stiffness. Osteoarthritis affects only joint functions unlike rheumatoid arthritis, in which the immune system attacks the tissues of the joints, erodes the lining on the joints causing inflammation, swelling, pain and deformity.
How does osteoarthritis occur?
All our joints are covered by a tough but slippery tissue that covers the ends of bones where they meet to form the joint. Healthy cartilage apart from absorbing shock during physical movement, allows our bones to glide smoothly over one another. Osteoarthritis, occurs when the surface layer of cartilage to breaks and erode away and the body is not able to repair joint tissue in the usual way.
Without the protective cartilage, the bones at the joints rub together against each other, which causes pain, swelling, and loss of normal shape and motion of the joint. Small pieces of bone or cartilage can also break off and float within the joint space which causes more pain and damage.
In addition, small deposits of bone which are called osteophytes may grow on the edges of the joint.
Who is prone to osteoarthritis?
Some people are more prone to osteoarthritis than others. They include:
- Women above the age of 45 years
- People with a family history of osteoarthritis
- People who are above 50 years
- People who have suffered from joint injuries
- People who are obese since the obesity puts increased stress and strain on the joints
- People with jobs that are physically strenuous such as those involves too much walking, weight lifting, kneeling or squatting for many hours at a stretch
- People with a poor posture
- Existing medical conditions such as osteonecrosis, Paget’s disease of bone, diabetes, gout, thyroid disorder
- People who lead a sedentary life
- People who are highly stressed
What are the causes of osteoarthritis?
Many factors can increase your risk of osteoarthritis such as:
- Ageing: It is seen that people older than 50 years are prone to osteoarthritis, which could be due to the muscles weakening and the body’s inability to heal itself as it did in younger years.
- Gender: Since women are more susceptible to injuries, they are more prone to osteoarthritis than men. In fact, the rate of osteoarthritis in women shoots up after menopause.Therefore experts believe that the female hormone estrogen must affect arthritis risk.
- Vitamin D Deficiency: People with a lower level of vitamin D intake have a higher risk of osteoarthritis.
- Vitamin C Deficiency: In people suffering from Vitamin C deficiency it is observed this condition progresses faster.
- Sudden changes in the weather: People with osteoarthritis are very sensitive to cold and damp weather.
- Hormones: the rate of osteoarthritis in women shoots up after menopause.Therefore experts believe that the female hormone estrogen is connected with arthritis risk. Women also experience much more severe knee osteoarthritis after menopause.
- Previous Joint Injuries: People with previous joint injuries are more prone to osteoarthritis
- Other Medical Conditions: Sometimes osteoarthritis is a result of damage from a different kind of joint disease, such as rheumatoid arthritis or gout.
- Lack of Exercise: People who lead a sedentary life are at a high risk of osteoarthritis.
- Obesity: Obesity can cause osteoarthritis since the joints are under increased strain.
What are the symptoms of osteoarthritis? How is osteoarthritis diagnosed?
The symptoms of osteoarthritis are:
- Joint aching and soreness, especially with movement
- Pain after overwork or after long periods of inactivity
- Stiffness in the joints after periods of rest particularly in the hips, knees, and lower back
- Bony enlargements in the middle and end joints of the fingers
- Joint swelling
- Clicking or cracking sound when a joint bends
- Pain that is worse after activity or toward the end of the day
Osteoarthritis affects different parts of the body in different ways, such as:
- Hips: Pain is felt in the groin area or buttocks and sometimes on the inside of the knee or thigh.
- Knees: A “grating” or “scraping” sensation is felt when moving the knee. Sometimes the grating sound is also heard.
- Fingers: Bony growths (spurs) at the edge of joints can cause fingers to become swollen, tender and red. There may be pain at the base of the thumb.
- Feet: Pain, tenderness, and stiffness are felt in the large joint at the base of the big toe. Swelling may also occur in the ankles or toes.
Diagnosis
Your primary care doctor or a general physician can diagnose osteoarthritis based on your symptoms, a physical exam, and some tests. He can also prescribe the medications. However, if your condition is too severe he will refer you to a rheumatologist or an osteopathic physician.
During the physical exam your doctor will check for:
- joint tenderness
- creaking or grating (crepitus) sounds
- bony swelling
- excess fluid
- reduced movement
- joint instability
- muscle thinning
He may suggest the following tests for confirmation:
- Blood tests – to help rule out other types of arthritis.
- X-rays – which can display bony spurs or narrowing of the space between your bones. They’ll also show whether any calcium has settled in your joint.
- Magnetic resonance imaging (MRI) scans – Rarely, an MRI scan of your knee can be helpful. This will show the soft tissues such as, cartilage, tendons, and muscles and changes in your bone that can’t be seen on a standard x-ray.
What are the complications of osteoarthritis?
The complications of osteoarthritis include:
- Complete breakdown of cartilage resulting in loose tissue material in the joints
- Bone death, also known as osteonecrosis
- Stress fractures
- Bleeding inside the joints
- Infection in the joints
- Rupture of the tendons and ligaments around the joint
- Pinched nerve (in the spine)
What is the treatment for osteoarthritis?
Medical Treatment for Osteoarthritis
Based on your condition the doctor may prescribe painkillers and anti-inflammatory medicines. In severe cases, the doctor may ask you to undergo joint surgery that can repair or replace severely damaged joints, especially hips or knees.
He may also suggest you undergo occupational therapy.
Exercise
Exercising is very beneficial for people suffering from osteoarthritis. It is advisable to consult your doctor before deciding on an exercise regimen since your doctor will be able to guide you on which exercises suit you the most.
Three kinds of exercise are important for osteoarthritis patients:
- exercises involving a range of motion also called flexibility exercises which include stretching the joints through their full span
- endurance or aerobic exercises which can strengthen your heart
- strengthening exercises to improve your muscle strength
Questions answered by trusted doctors

Did you know?
Leading cause of disability among older adults
Osteoarthritis is a leading cause of disability in people over 50 years of age.
Most prevalent form of arthritis
Osteoarthritis is the most prevalent form of arthritis in India, affecting over 15 million adults every year
Osteoarthritis capital
India may become the osteoarthritis capital of the world with over 60 million cases by 2025, doctors say.
Related videos
Related articles
Asthma is a chronic lung condition caused by inflammation and narrowing of the bronchial tubes. Read about the symptoms, treatment, cure and remedies of Asthma. Get information, videos and facts about Asthma on Health-Wiki | Practo
The treatment method of using various treatments like chemotherapy, radiation, anti-cancer drugs to either cure, treat, control, or reduce the symptoms of any types of cancer can be grouped together as cancer treatments.
Irritable bowel syndrome is a functional disorder of the bowels which leads to the occurrence of a group of symptoms. Know more about Irritable bowel syndrome, its causes, symptoms, treatment and other useful facts and videos on Health-Wiki | Practo

Drugs to heal the wear and tear of joint, drugs to control pain ,if osteoarthritis is severe joint replacement, consult orthopedic surgeon get evaluated
In OA, cartilage gets eroded due to various reasons. Cartilage doesn't have the capacity to heal. As a result, there are no medications that can bring it back to normal. There are many supplements but when body doesn't heal the cartilage, it's very doubtful if these supplements will work at all.
Avoiding activity even if you did have arthritis is not a very good idea. The best way to deal with arthritis is to replace impact activities with non-impact activities like cycling or swimming. If at all you want to do running use the bare foot running technique. Activity will also help keep your weight under control. In terms of diet, reduce all white substances like rice, sugar, sweets. Replace with brown food like oats, muesli or brown bread, and plenty of salads and fruits.
Osteoarthritis is not curable. You can avoid further wear and tear of the cartilage by keeping your weight under control, staying active and being flexible. If you are playing any sports then avoid playing sports like football or basketball. Badminton or tennis played gently are good.
Lastly who has diagnosed you with arthritis and how has this diagnosis been reached? It may be just a flare up of cartilage irritation.
Hope this helps.
Dr Vinu Raj
Consultant Orthopaedic Surgeon
MBBS MRCS FRCS(Trauma&Orth)
https://play.google.com/store/apps/details?id=com.technoherpes.kneepain
Or you can search " knee pain relieving exercises by Dr kavin khatri" on google playstore