Contents
In this article we will look at:
- What is premenstrual syndrome?
- How does premenstrual syndrome occur?
- Who is prone to premenstrual syndrome?
- What are the causes of premenstrual syndrome?
- What are the symptoms of premenstrual syndrome?
- When to see a doctor for premenstrual syndrome?
- What are the complications of premenstrual syndrome?
- What is the treatment of premenstrual syndrome?
You can click on any of the links above to navigate to the section of your interest.
What is premenstrual syndrome?
Premenstrual syndrome is a group of emotional, physical, mental, and behavioural disturbances experienced by a woman before her menstrual cycle. Approximately 85 % of the women in this world experience PMS. Most of the women experience at least one symptom of PMS every month, prior to menstruation.
These symptoms occur in a woman around two weeks before her monthly period (i.e. during her period of ovulation). The signs become more intense 2-3 days prior to the period, and usually resolve a day or two after the period commences.
How does premenstrual syndrome occur?
PMS can affect menstruating women of any age, and the effect is different for each woman. For some women, the symptoms can vanish as soon as menstruation starts. For others, it can be so severe that it makes it hard to even get through the day. For these women, the PMS symptoms subside once the menstruation stops. Women stop experiencing PMS when they are pregnant or once they reach menopause. Women who have undergone hysterectomies can experience PMS every month even if at least one functional ovary is left.
How or why PMS symptoms occur is not clear, but several factors may be involved. Changes in hormones which can result in chemical changes in the brain, during the menstrual cycle, seem to be an important cause. Hormonal level changes may affect some women more than others. Other issues such as stress and emotional problems, such as depression, may make PMS symptoms worse.
Other possible causes can include:
an unhealthy diet resulting in low vitamins and minerals for the body
obesity
heavy smoking or alcohol drinking
too much of caffeine intake
leading a sedentary life
These factors can cause PMS symptoms such as anxiety, irritability, fatigue, depression, headache, back pain, food cravings, acne, swollen tender breasts, stomach bloating, constipation or diarrhea.
Who is prone to premenstrual syndrome?
Women who are at an increased risk of suffering from PMS :
have a family history of PMS
lead a sedentary lifestyle
take an unhealthy diet
drink a lot of alcohol
smoke heavily
are below 30 years of age
consume a high sugar diet
have more than two children
suffer from high-stress levels
take a diet low in vitamin B, calcium, and magnesium
do not exercise
are prone to take a lot of caffeine
What are the causes of premenstrual syndrome?
The causes of PMS have not yet been established.
Researchers, however, believe that:
Hormonal changes can cause PMS: A change in the hormones during the menstrual cycle can cause PMS. Levels of oestrogen and progesterone hormones rise and fall just prior to, and during a menstrual cycle. An increase in these hormones can cause mood swings, anxiety, and irritability.
Chemical changes in the brain can cause PMS: The change in hormones can also affect certain chemical levels in the brain. For instance, serotonin which can regulate our moods and make us happier may reduce with a change in the hormone level. This can directly affect our moods.
- Physical and lifestyle factors can cause PMS: It has been observed that obese women are more likely to have PMS. Other lifestyle factors such as an unhealthy diet, heavy smoking and drinking, or too much stress can also cause PMS.
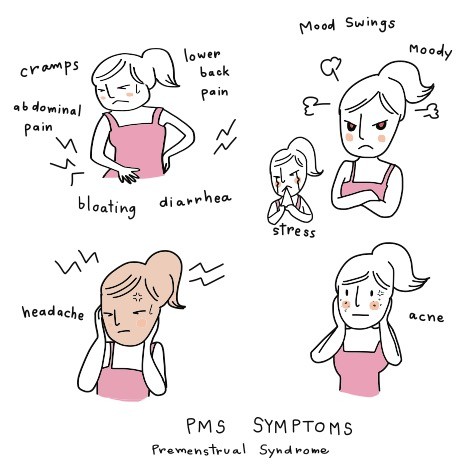
What are the symptoms of premenstrual syndrome?
The symptoms of premenstrual syndrome are:
acne
joint or muscle pain
trouble with concentration or memory
anxiety, irritability, mood swings
swollen or tender breasts
constant fatigue
insomnia
bloated abdomen
abdominal pain or cramps
constipation or diarrhea
headache or backache
appetite changes or food cravings
sadness
When to see a doctor for premenstrual syndrome?
You need to visit a doctor if any of your symptoms especially your mood swings, depression, or abdomen, joint and muscle pains are interfering with your day to day activities, or if they do not go away even after menstruation has stopped.
Recurrent symptoms can also occur due to an underlying disorder such as:
chronic fatigue syndrome
rheumatic disorders
What are the complications of premenstrual syndrome?
The complications of PMS include:
severe anxiety
thoughts of suicide
severe mood swings
substance abuse due to severe depression
existing medical conditions such as migraines, asthma, seizure disorders, multiple sclerosis, systemic lupus erythematosus, inflammatory bowel disease, and irritable bowel syndrome (IBS) may exacerbate
trouble thinking or focusing
painful cramps
lack of interest in daily activities
extreme anger
What is the treatment of premenstrual syndrome?
Medical Treatment
Many women experience relief from PMS symptoms through lifestyle changes alone. For aggravated cases though, your doctor may prescribe medicines for the symptoms such as:
antidepressants
nonsteroidal anti-inflammatory drugs
diuretics
hormonal contraceptives
painkillers
oestrogen-only patches and implants
Exercise
Exercising regularly can help you to get complete relief from PMS symptoms. Doing aerobics at least for two hours per week can help alleviate the symptoms. Other activities can include brisk walking, swimming, and cycling. These activities will help keep depression at bay.
Stretching and breathing exercises, such as yoga and pilates, will help reduce your stress levels.
Questions answered by trusted doctors

Did you know?
Fatigue is a common symptom
The most commonly reported PMS symptom in India is 'fatigue/lack of energy' (68.3%), followed by 'decrease interest in work' (60.1%) and 'anger/irritability' (59.9%).
Poor health leads to PMS
PMS is associated with poor physical health and existing psychological distress.
Healthy lifestyle key to preventing PMS
A healthy lifestyle consisting of healthy diet and proper physical exercise is the first step to preventing and managing PMS.
Related videos
Related articles
Polycystic Ovary Syndrome (PCOS) is a common endocrine disorder among women of child-bearing age. Know more about the symptoms, treatment, cure, and remedies of PCOS. Get information, videos and facts about PCOS on Health-Wiki | Practo
The treatment method of using various treatments like chemotherapy, radiation, anti-cancer drugs to either cure, treat, control, or reduce the symptoms of any types of cancer can be grouped together as cancer treatments.
Dialysis is a procedure in which the blood is filtered mechanically without the help of the kidneys. If the kidneys are not functioning properly then Dialysis will take over the function of the failed kidneys.



Kindly suggest what would be the problem