Contents
In this article, we will take a look at:
- What is cholelithiasis?
- How does cholelithiasis occur?
- Who is prone to cholelithiasis?
- Symptoms of a cholelithiasis
- Diagnosis of a cholelithiasis
- Complications of a cholelithiasis
- Treatment for a cholelithiasis
You can click on any of the links above to navigate to the section of your interest.
What is Cholelithiasis?
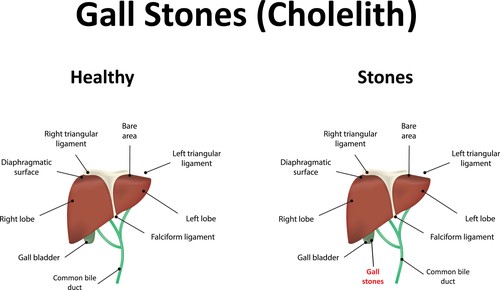
Cholelithiasis is a medical condition where hard, pebble-like deposits develop within the gallbladder of an individual. They are also known as gallstones. These stones can be as small as a grain of sand or as large as a golf ball. The gallbladder is a small organ present in the abdominal cavity of human beings whose function is to store the bile. When stones develop within this organ, it may give rise to excruciating pain along with jaundice. Treatment is essential immediately after detection as gallstones may lead to severe complications.
There are two types of gallstones or cholelithiasis
Cholesterol Stones
The most prevalent kind, approximately 80 per cent of all gallstones fall into this category. They are made of cholesterol and are yellow-green.
Pigment Stones
Also called bilirubin stones, these stones are made of bilirubin, and they mostly develop at the time of haemolysis (destruction of red blood cells). They are dark brown or black.
How does Cholelithiasis occur?
The exact cause for the occurrence of cholelithiasis has not been determined. Recent studies hint that the presence of excess cholesterol in the blood may be responsible for the formation of cholesterol stones. When bile in the liver cannot dissolve excess cholesterol, it develops into gallstone.
Similarly, the pigment stones develop as a result of abundant bilirubin in the body. Specific conditions like liver damage or blood disorders lead to the formation of excess bilirubin which the gallbladder is unable to break down. It may result in the development of hard, dark coloured pigment stones within the gallbladder.
Who is Prone to Cholelithiasis?
The risk of developing cholelithiasis increases manifold if:
- Your age is above 40 years.
- You have a family history of cholelithiasis.
- You have undergone an organ transplant or bone marrow transplant.
- You are diabetic.
- You have cirrhosis of the liver.
- You have undergone bariatric surgery and have experienced excessive weight loss as a result of it.
- You have medical conditions like haemolytic anaemia and sickle cell anaemia.
What are the Symptoms of Cholelithiasis? How is Cholelithiasis Diagnosed?
The symptoms of cholelithiasis include:
- Pain on the right side of the upper abdomen.
- Nausea and vomiting.
- Fever.
- Jaundice.
- Dark coloured stools.
- Dark coloured urine discharge.
- Diarrhoea.
In some cases, when cholelithiasis does not produce any symptoms, its known as “silent gallstones” or “asymptomatic cholelithiasis.” The pain occurs when these gallstones block the pathway of the cystic duct or common bile duct. This condition is also known as biliary colic. In 80 per cent of the cases, gallstones remain asymptomatic. The patient remains unaware of this condition until it gets detected through X-Ray at the time of routine health analysis.
Diagnosis
In most of the cases, cholelithiasis gets diagnosed at the time of routine health check-up through X-Rays and lower abdomen ultrasound examination. However, if the patient experiences sharp pain in the middle to the upper abdomen, the doctor performs a physical exam to detect abnormalities in the physical characteristic of the body. If he notices a yellow tint on the skin and in the eyes, he diagnostic tests like ultrasound examination, abdominal CT scan, gallbladder radionuclide scan and Endoscopic retrograde cholangiopancreatography (ERCP). All these tests help in the confirmation or ruling out of cholelithiasis in patients. The gallbladder radionuclide scan helps to find out whether there is an infection or blockage associated with the cholelithiasis.
What are the Complications of Cholelithiasis?
If left untreated for a prolonged period, gallstones may lead to severe complications like:
Acute Cholecystitis
Here the gallstones block the cystic duct which supplies the bile juice from the gallbladder. It results in inflammation, infection, along with excruciating pain in the abdominal region. Approximately 1-3 per cent of patients having gallstones may develop cholecystitis in the future.
Other complications of cholelithiasis include sepsis (infection in the blood), gallbladder cancer, cholangitis (a disorder in the gallbladder), fever, chills, jaundice, pain in the abdomen, and appetite loss.
What is the Treatment for Cholelithiasis?
If Cholelithiasis becomes symptomatic, surgery is the best treatment. This process is known as a cholecystectomy. Earlier, surgeons usually performed open cholecystectomy or removal of the entire gallbladder to eliminate the stones. Nowadays, laparoscopic cholecystectomy is a more common course of treatment. Some doctors also use chemicals like chenodeoxycholic acids (CDCA) or ursodeoxycholic acid (UDCA, ursodiol) to dissolve the gallstones and flush it out through urine. However, a higher probability of recurrence of cholelithiasis exists, and this treatment takes a longer time to show effective results.
Questions answered by trusted doctors

Did you know?
Regular exercises and yoga
Regular exercises and yoga help to prevent the occurrence of gallstone.
Rapid weight loss treatment
Rapid weight loss treatment and individuals undergoing bariatric surgery have a higher risk of developing cholelithiasis in the future.
The non-surgical method of gallstone removal
The non-surgical method of gallstone removal in aged patients involves the use of electrohydraulic shock wave lithotripsy (ESWL).
Related articles
Nausea is the uneasiness one feels in the stomach, just before one feels the urge to vomit. Find out about nausea medicine, symptoms, remedies. Get information, videos and facts about nausea on Health-Wiki | Practo
Phimosis is a health condition in which the foreskin is not retracted or pulled back from around the tip of the penis.
Lung diseases are those that affect either the whole of or different parts of the lungs and their linings. These cause difficulties in breathing and related complications.
You can easily take an online consultation for further treatment guidance and permanent cure without any side effects
Medicines will reach you via courier services
Cholecystitis can become very severe and in most cases requires immediate medical attention. See your doctor as soon as possible if you think you have acute cholecystitis.
This condition can become chronic if it persists for a prolonged period of time, or if you’re having recurring symptoms from the inflammation.
Cause:
Gallstones are by far the most common cause of acute cholecystitis. Bile can build up in the gallbladder if gallstones obstruct the bile ducts. This leads to inflammation.
Acute cholecystitis can also be caused by a severe illness or a tumor. However, these causes are rare.
The condition is considered chronic when attacks of cholecystitis are repeated or prolonged.
Women get gallstones more often than men. They also have a higher risk of developing acute cholecystitis.
Risk increases with age in both men and women, although the reason for this is unclear. The risk is also higher for people of Scandinavian, Native American, or Hispanic descent.
SYMPTOMS:
The most common sign that you have acute cholecystitis is abdominal pain that lasts for several hours. This pain is usually in the middle or right side of your upper abdomen. It may also spread to your right shoulder or back.
Pain from acute cholecystitis can feel like sharp pain or dull cramps. It’s often described as excruciating.
Other symptoms include:
Clay-colored stool
Vomiting
Nausea
Fever
Yellowing of your skin and the whites of your eyes
pain, typically after a meal
Chills
Abdominal bloating.